A hip fracture is a partial or complete break of the upper femur (thigh bone) in or near the hip. Hip fractures are most common in people older than 60 whose bones have been weakened by osteoporosis. Most of those fractures result from falls.
A fractured hip is usually very painful, and the potential for complications in older patients means that immediate surgery is generally the recommended treatment. The sooner a patient can be treated and gotten out of bed, the better the outcome is likely to be.
Complications of hip fracture in the elderly may include:
- Bed sores
- Blood clots
- Pneumonia
- Disorientation in very old patients on prolonged bedrest, which makes rehabilitation and recovery much more difficult.
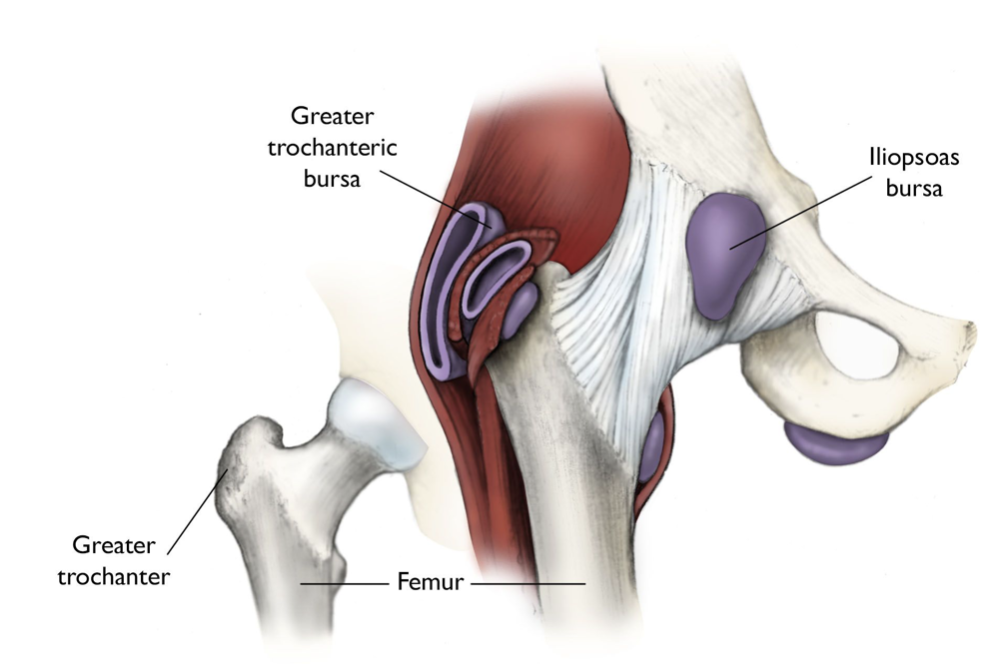
Anatomy
The hip is a ball-and-socket joint. The femoral head is known as the ball and is located at the top of the femur or thigh bone. The acetabulum is the socket and is part of the pelvis. When we are discussing a hip fracture, we are referring to a partial or complete break of the upper femur.
There are four areas of the upper femur where a hip fracture may occur:
- Femoral head. The ball that is the upper end of the femur.
- Femoral neck. The area between the femoral head and the intertrochanteric area.
- Intertrochanteric area. The area between the femoral neck and the shaft of the femur is characterized by two bony landmarks: the greater trochanter and the lesser trochanter
- Subtrochanteric area. The upper part of the femur shaft, below the greater and lesser trochanters.
Most hip fractures happen in the femoral neck and intertrochanteric area.
Cause
Most hip fractures in the elderly are the result of “low energy” falls. A low energy fall is defined by the World Health Organization as “forces equivalent to a fall from a standing height or less”. A fall like this would be extremely unlikely to injure a younger person, but when combined with weak or brittle bones, such a fall can be very damaging to older people.
The elderly are also susceptible to spontaneous fracture, where the break happens as a result of twisting or bending and may actually cause a fall. Spontaneous fractures tend to occur in the femoral neck. 70 percent of all hip fractures occur in post-menopausal women, as diminished estrogen levels contribute to greater loss of bone tissue.
Symptoms
A hip fracture is acutely painful. The pain is usually localized in the groin or upper thigh, but that’s not always the case. Other symptoms may include:
- Hip/knee pain
- Lower back pain
- Inability to stand or walk
- Bruising/swelling
- Foot turned out at an odd angle making the leg look shorter
Treatment
It is rare for a hip fracture to be considered stable, meaning it will not displace if the patient is allowed to sit. If the fracture seems stable, the patient may be treated without surgery, but the age and overall health of the patient and the possible complications of extended bedrest must be considered in that decision.
If the break occurred in the femoral neck, 1-3 metal pins are used to hold the two pieces of fractured bone together. The procedure is relatively simple, and patients may begin putting weight on the leg right after surgery.
If the break occurred in the intertrochanteric area, it’s likely to be the result of a fall and there may be multiple broken bones. A plate and screws may be needed to align and hold the broken pieces together as they heal. The muscles will create compression to help hold the bone in place.
If the femoral head has been displaced, it’s likely the blood supply to the bone is compromised, and avascular necrosis may occur, causing the bone of the femoral head to collapse and die. Hip replacement surgery is then necessary.
Prevention
It’s always easier to prevent a problem than to have to fix it. Falls are the most common cause of hip fracture, so the first thing to do is identify and fix – or mitigate – the hazards:
- Exercises that help improve balance and gait
- Taming loose rugs, electrical cords, and slippery surfaces
- A diet rich in calcium and vitamin D
- Prescription medications if necessary
- Assistive devices (walker, cane, grab bars) if necessary